By Elizabeth Boudrie
Back in 2010, when the Patient Protection and Affordable Care Act (PPACA), better known to many as Obamacare, was newly minted, we undertook a research project in cooperation with the ADP Research Institute to get a sense of employers’ familiarity with, preparedness for, and impressions of the main provisions of PPACA. At that time, given the political climate, we were unsure if PPACA would actually live to be implemented.
Fast forward to today. In light of more recent events—the Supreme Court’s ruling to uphold PPACA, and President Obama’s recent reelection—we thought we would revisit those research findings. For our survey, we received responses from a total of 680 senior executives in small (1 to 49 employees), mid-size (50 to 999), and large (1,000+ employees) United States-based, private sector (non-government) organizations. We analyzed the results based on these categories, given that impacts of these provisions vary by organization size. We reviewed respondents’ anticipated impact on HR staffing caused by the implementations of PPACA.
In particular, our review of the findings focused on two key provisions of the legislation.
Provision: Requirement to offer coverage or pay a penalty. This provision essentially requires employers with 50 or more employees either to offer healthcare coverage or pay a penalty. Implementation starts in 2014.
There is an anticipated impact on benefits offerings. The vast majority of employers of all sizes that already offer health insurance coverage to their full-time employees are likely to continue to do so post implementation: 90 percent, 91 percent, and 96 percent of small, mid-size and large employers, respectively, say they are likely to continue offering benefits.
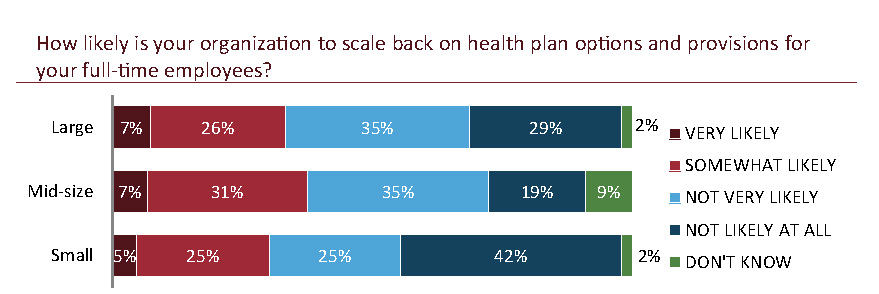
The scale of those benefits, however, may change. Just about a third of employers (30 percent of small; 38 percent of mid-size; 33 percent of large) say they are likely to scale back health plan options and benefits as a result of the implementation of PPACA.
Among those employers that do not currently offer healthcare coverage to their full-time employees, the impacts of this provision on benefits offerings vary by employer size. This issue is relevant to small and mid-size employers only; all of the large employer respondents already offer this coverage. A minority of small employers (11 percent) say they are likely to begin offering healthcare coverage to their employees (and, of course, given their size, they won’t be required to do so), versus 66 percent who say they are unlikely to do so. The remainder are unsure. On the other hand, 31 percent of mid-size employers say they are likely to begin offering healthcare coverage to their employees, while 38 percent say they are unlikely to do so, even though many (based on their size) would be impacted by this provision. The remaining 31 percent of this group are unsure.
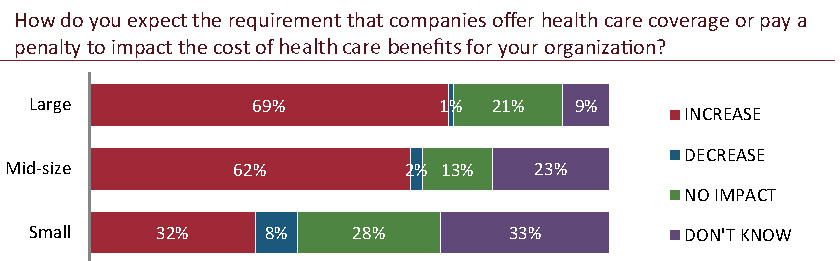
There is also an anticipated impact on benefits cost. Mid-size and large employers most often anticipate an increase in benefits cost as a result of the implementation of this provision of PPACA, with 62 percent of mid-size and 69 percent of large employers anticipating an increase. While 32 percent of small employers anticipate a cost increase as a result of this provision, almost the same amount (33 percent) are unsure of the benefits cost implications of this provision.
Among those employers that anticipate an increase in costs, small and mid-size employers most often expect an increase of between 11 percent and 20 percent, while large employers anticipate a smaller increase of 10 percent or less.
Each employer size group has a different impression of the impact of this provision on compliance costs. Small employers, because they recognize that this provision does not apply to them, most often say there will be no impact on their compliance costs. However, more than a quarter are unsure, and 17 percent do anticipate some level of compliance cost increase.
Mid-size employers also most often anticipate no impact on compliance costs as a result of the implementation of this provision of PPACA. That said, 39 percent anticipate some level of cost increase, most often minimal—an increase of 5 percent or less. Large employers most often anticipate a compliance cost increase as a result of this provision of the PPACA, generally of 5 percent or less.
Provision: “Cadillac” health plan tax. This provision imposes a tax on insurers of employer-sponsored “Cadillac” plans whose aggregate value exceeds $10,200 for individual coverage and $27,500 for family coverage. Implementation starts in 2018.
Impact on benefits offerings
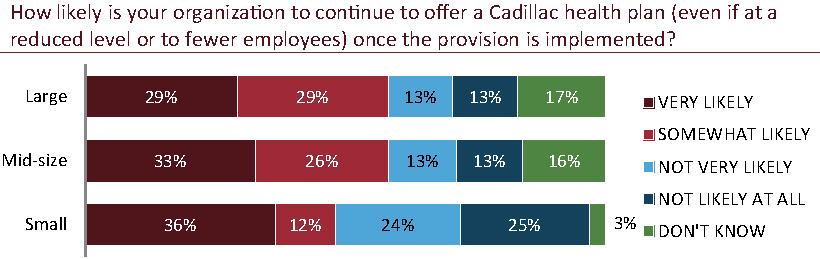
Small employers that already offer Cadillac health plans are just about as likely to continue doing so as not (48% say they’ll continue; 49% say they’ll discontinue). Mid-size and large employers, on the other hand, are more likely to continue these plans, with just over half of each group saying they are likely to do so.
However, among those employers that are likely to continue to offer Cadillac plans, smaller employers are less likely to scale back than their mid-size and larger counterparts, with 24% of small employers saying they are likely to scale back versus 43% and 93% of mid-size and large employers, respectively.
Impact on benefits costs
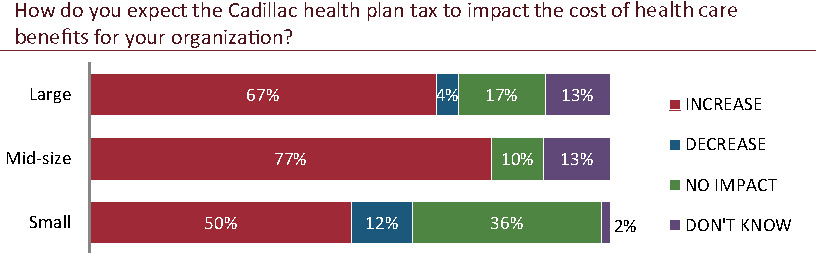
The highest percentage of each employer size group anticipates a cost increase as a result of this provision of PPACA. Here again, among those employers that anticipate an increase in costs, small and mid-size employers most often expect an increase of between 11 percent and 20 percent, while large employers expect that increase to be 10 percent or less.
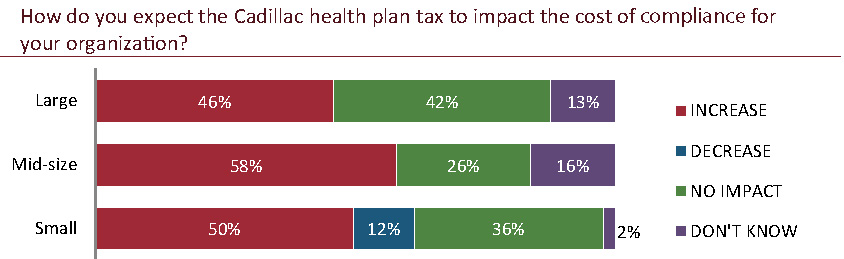
Impact on compliance costs
The highest percentage of all three groups say they anticipate a compliance cost increase as a result of the implementation of this provision of PPACA. Opinions vary as to the amount of increase, with small employers most often anticipating the highest increase (an increase of more than 20 percent), mid-size employers most often expecting between 6 percent and 10 percent increase and large employers most often anticipating an increase of 5 percent or less.
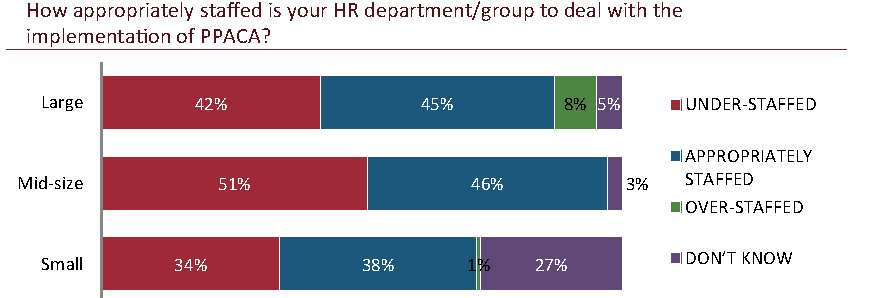
Staffing and PPACA
The different employee size groups have varying reactions as to the appropriateness of their staff levels to deal with the implementation of PPACA. While both the small and large employer sets are most likely to say they are appropriately staffed (38 percent and 45 percent respectively), more than a quarter of small employers don’t know if they are appropriately staffed or not. And, nearly as many in both size groups say they are under-staffed (34 percent small; 42 percent large).
The mid-size employers’ results are reversed: the highest percentage (51 percent) says they are under-staffed, while 46 percent say they are appropriately staffed.
With the upcoming implementation of some of the more impactful provisions, HRO Today magazine (in a monthly feature) and the HRO Today Institute (in its ongoing research efforts) will continue to explore the impacts of healthcare legislation on the HR community.
Elizabeth Boudrie is executive director of the HRO Today Institute and vice president of research for SharedXpertise.